Authored By: Crystal Baker, MPH Student
Crystal is an MPH student at Youngstown State University. She has experience working with various non-profit organizations, focusing on community health, advocacy, and program coordination. Her work often involves addressing social determinants of health and fostering collaboration to support health equity and access. As part of her capstone with CTRC, she is gathering data to develop prescriptive guidelines for providers on the role of digital health tools during disasters.
As climate change intensifies and the frequency of natural disasters increases, healthcare systems must evolve to overcome challenges brought forward by these issues. Digital health tools, including telehealth, artificial intelligence (AI), and remote monitoring technologies, can be a vital tool in disaster preparedness, mitigation, and recovery. This blog post presents insights from an environmental scan that explores how these modalities can be effectively leveraged in disaster contexts.
Key Takeaways from Literature Review
Of the 11 articles included the main points included:
- Increased Usage of DHT: There was a rise in telehealth modalities, including video/audio calls, audio-only visits, and patient-to-provider messaging during disasters (Uscher-Pines et al., 2018; Baek et al., 2021).
- Maintaining Regular Care: Telehealth visits primarily addressed the routine needs of new users rather than new issues stemming from the disaster, focusing on medication refills and general medical advice (Uscher-Pines et al., 2018; Baek et al., 2021).
- Prevention of Health Decline: Access to telehealth, particularly in the critical weeks following a disaster, can help prevent worsening health conditions and avoidable hospitalizations (Friedman, 2022).
- Communication and Access: Messaging systems were utilized to keep patients informed about operational healthcare facilities and to assist in rescheduling appointments, effectively reducing barriers to care (Baek et al., 2021).
- Reduction of ER Visits: The implementation of telehealth and store and forward messaging significantly decreased unnecessary post-disaster emergency room visits, showcasing the effectiveness of these modalities in managing patient care (Friedman et al., 2022).
- Support for In-Person Providers: The review highlighted live eConsults, emphasizing their role in adhering to clinical protocols and improving care quality (Armaan et al., 2021). Remote synchronous econsultations facilitated access to specialists, enhancing the support provided to in-person care teams by verifying dosages and offering consultations (Boyle et al., 2023; Armaan et al., 2021).
Supplemental findings included:
- Identification of Barriers: The review highlighted various barriers and disparities in accessing digital health technologies (DHT), emphasizing the need for improvements in credentialing and support systems.
- Older Adult Utilization: Older adults successfully utilized remote health technologies, indicating that these tools can effectively assist populations with limited in-person interaction during emergencies (Der-Martirosian, 2020).
- Training and Preparedness: Providing targeted training during preparedness phases can enhance older adults’ ability to use telehealth services, ensuring they are equipped with the necessary knowledge and support when emergencies arise (Der-Martirosian, 2020).
- Focus on Vulnerable Populations: Given that telehealth users are often older and medically vulnerable, improving accessibility and utilization through targeted training and education is crucial for these high-risk groups.
- Support for eConsults: While eConsults were widely supported among providers, there remains a need to explore frameworks that facilitate synchronous eConsults and develop standardized policies for disaster credentialing (Boyle, 2023).
- Linking Preparedness with Mitigation and Recovery: Although few articles focused specifically on preparedness, many mitigation and recovery strategies were rooted in preparedness principles. Establishing the necessary infrastructure, education, and tools during preparedness phases is essential for effective use of DHT during disasters.
Application by DHT Modality
Modality |
Applications |
| Telehealth |
Reduce demands in ER and Hospital by treating not urgent or minor issues remotely during disasters Suitable for complicated/high-risk patients or those with various barriers (transportation, destroyed roads, etc) but must have access to internet |
| Asynchronous store and forward (patient to provider messaging) |
Reduce demands in ER and Hospital by treating not urgent or minor issues remotely during disasters Aid in rerouting and rescheduling patients Provide updates on office operations and the impact of disasters |
| Asynchronous and synchronous eConsult |
Reduce errors or help with supplemental tasks (verifying dosage) as demands are increased and resources are resources Reallocate workforce resources from areas not impacted by disaster |
Challenges
As DHT is increasingly being utilized, challenges have arose. The systematic review reviewed the following challenges:
- Demographic Disparities: Socioeconomic factors lead to disparities in telehealth access, with Black patients being less likely to engage in telehealth visits compared to White patients (Brotman et al., 2021; Hall et al., 2021). This inequity can hinder equitable care during natural disasters.
- Infrastructure Vulnerabilities: Disasters can exacerbate infrastructure issues, such as power outages and inadequate internet connectivity, which significantly affect the utilization of digital health technologies. Addressing these challenges is crucial for effective deployment during disasters (Baek et al., 2021).
- Technological Limitations: Limited digital literacy among populations can impede the effective use of digital health technologies, emphasizing the need for education and support in disaster preparedness and response.
- Need for Climate-Resistant Infrastructure: Some literature highlights the importance of climate-resistant infrastructure but lacks specific examples or strategies for improving resilience, particularly regarding internet and electricity access for lower socioeconomic groups.
- Credentialing Issues: The absence of standardized credentialing processes for telehealth providers, particularly for modalities like eConsults, poses significant challenges in maintaining consistent quality of care (Boyle, 2023). Inconsistent protocols can lead to delays in service delivery, especially during disasters when rapid deployment is necessary (Boyle, Ludy, et al., 2023).
- Acceptance and Usability: Despite high acceptance of digital health technologies among providers and patients, there is a demand for simpler, more reliable technology interfaces with improved audiovisual quality, particularly for low-frequency, high-stakes scenarios (Boyle, Ludy, et al., 2023).
Literature Review Overview and Abstract
INTRODUCTION: Climate change is increasing the frequency of natural disasters, which disrupt critical infrastructure and healthcare delivery, highlighting the need for more climate-resilient healthcare systems. This review explores how digital health technologies (DHTs) can be utilized by healthcare providers to maintain patient care during disasters, focusing on effective modalities and the challenges of implementing DHTs in emergency scenarios.
METHODS: A structured review was conducted using databases including PubMed Central, JMIR, and Science Direct, focusing on peer-reviewed articles published in the last 10 years that examined digital health technologies used during natural disasters. Data extraction and bias assessments were performed on eligible articles to ensure quality and reliability.
RESULTS: The search yielded 1,834 records from three databases, and after screening titles, abstracts, and full texts, 11 studies met the inclusion criteria. These studies consisted of five qualitative, five observational, and one mixed-methods study. A bias assessment categorized the studies as one weak, four moderate, and six strong.
DISCUSSION: The review found that digital health technologies like telehealth, patient-provider messaging, and eConsults were crucial for maintaining care during disasters, reducing emergency visits, and improving care coordination. However, challenges such as infrastructure vulnerabilities, credentialing inconsistencies, and disparities in access, particularly for socioeconomically disadvantaged groups, highlight the need for improvements in preparedness and resilience planning.
LIMITATIONS: The review is limited by the small number of studies focused on disaster-specific digital health applications, potential publication bias, and the exclusion of non-English articles. Additionally, the lack of standardized terminology and protocols across DHT modalities makes comparisons and generalizations challenging.
RECOMMENDATIONS: The review recommends that providers use telehealth, patient-provider messaging, and eConsults during disasters to reduce strain on emergency services, manage minor health issues remotely, and provide real-time consultations. Training for both staff and patients on these tools prior to disasters is essential, along with the establishment of standardized protocols to ensure effective implementation and continued access to care.
Figure 1: PRISMA Flowchart
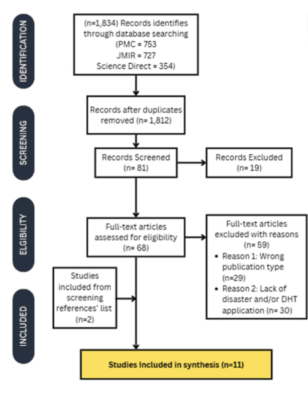
Full literature review COMING SOON
References
Baek, J., Simon-Friedt, B., Lopez, A., Kolman, J. M., Nicolas, J., Jones, S. L., Phillips, R. A., & Menser, T. (2021). Assessing patient needs during natural disasters: Mixed methods analysis of portal messages sent during Hurricane Harvey. Journal of Medical Internet Research, 23(9), e31264. https://doi.org/10.2196/31264
Boyle, T. P., Boggs, K., Gao, J., McMahon, M., Bedenbaugh, R., Schmidt, L., Zachrison, K. S., Goralnick, E., Biddinger, P., & Camargo Jr, C. A. (2023). Hospital-level implementation barriers, facilitators, and willingness to use a new regional disaster teleconsultation system: Cross-sectional survey study. JMIR Public Health and Surveillance, 9, e44164. https://doi.org/10.2196/44164
Boyle, T. P., Ludy, S., Meguerdichian, D., Dugas, J. N., Drainoni, M. L., Litvak, M., Bedenbaugh, R. T., Schmidt, L., Miller, K., Biddinger, P. D., & Goralnick, E. (2023). Feasibility and acceptability of a model disaster teleconsultation system for regional disaster health response. Telemedicine Journal and e-Health: The Official Journal of the American Telemedicine Association, 29(4), 625–632. https://doi.org/10.1089/tmj.2022.0103
Brotman, J. J., & Kotloff, R. M. (2021). Providing Outpatient Telehealth Services in the United States. Chest, 159(4), 1548–1558. https://doi.org/10.1016/j.chest.2020.11.020
Cybersecurity and Infrastructure Security Agency. (n.d.). Wildfires | CISA. Www.cisa.gov. https://www.cisa.gov/topics/critical-infrastructure-security-and-resilience/extreme-weather-and-climate-change/wildfires
Der-Martirosian, C., Heyworth, L., Chu, K., Mudoh, Y., & Dobalian, A. (2020). Patient characteristics of VA telehealth users during Hurricane Harvey. Journal of Primary Care & Community Health, 11, 2150132720931715. https://doi.org/10.1177/2150132720931715
Department of Homeland Security. (2018). Natural disasters. Department of Homeland Security. https://www.dhs.gov/natural-disasters man, R. S. C., Carpenter, D. M., Shaver, J. M., McDermott, S. C., & Voelkel, J. (2022). Telemedicine familiarity and post-disaster utilization of emergency and hospital services for ambulatory care sensitive conditions. Journal of Telemedicine and Telecare.
FEMA. (n.d.). Earthquake | National Risk Index. Hazards.fema.gov. https://hazards.fema.gov/nri/earthquake
Hall, K., Kafashzadeh, D., Chen, L., Dudovitz, R., & Ross, M. K. (2021). Trends in telemedicine visits among pediatric asthma patients during COVID-19. Journal of Telemedicine and Telecare.
He, S., Marzouk, S., Balk, A., Boyle, T., & Lee, J. (2022). The telehealth advantage: Supporting humanitarian disasters with remote solutions. American journal of disaster medicine, 17(2), 95–99. https://doi.org/10.5055/ajdm.2022.0423
Learmonth, Y. C., Assunta, H., Skeffington, P., Diana, W., Kermode, A. G., & Marck, C. H. (2023). Healthcare complexities during community crises: Recommendations for access to healthcare for Australians with multiple sclerosis. Journal of Healthcare Management.
Lokmic-Tomkins, Z., Bhandari, D., Bain, C., Borda, A., Kariotis, T. C., & Reser, D. (2023). Lessons Learned from Natural Disasters around Digital Health Technologies and Delivering Quality Healthcare. International journal of environmental research and public health, 20(5), 4542. https://doi.org/10.3390/ijerph20054542
Paschoalotto, M. A. C., Lazzari, E. A., Rocha, R., Massuda, A., & Castro, M. C. (2023). Health systems resilience: Is it time to revisit resilience after COVID-19? Health Systems.
Rowther, A. A., Mehmood, A., Razzak, J. A., Atiq, H., Castillo-Salgado, C., & Saleem, H. T. (2021). “You can only help them save the patient once they trust you”: Clinician perspectives and theories of the use of a pediatric emergency teleconsultation program. Journal of Telemedicine and Telecare.
Uscher-Pines, L., Fischer, S., Tong, I., Mehrotra, A., Malsberger, R., & Ray, K. (2018). Virtual first responders: The role of direct-to-consumer telemedicine in caring for people impacted by natural disasters. Journal of General Internal Medicine, 33(8), 1242–1244. https://doi.org/10.1007/s11606-018-4440-8







Leave a Comment